The Epidemic and Eradication Efforts of Malaria in Developing Countries


Contents Overview
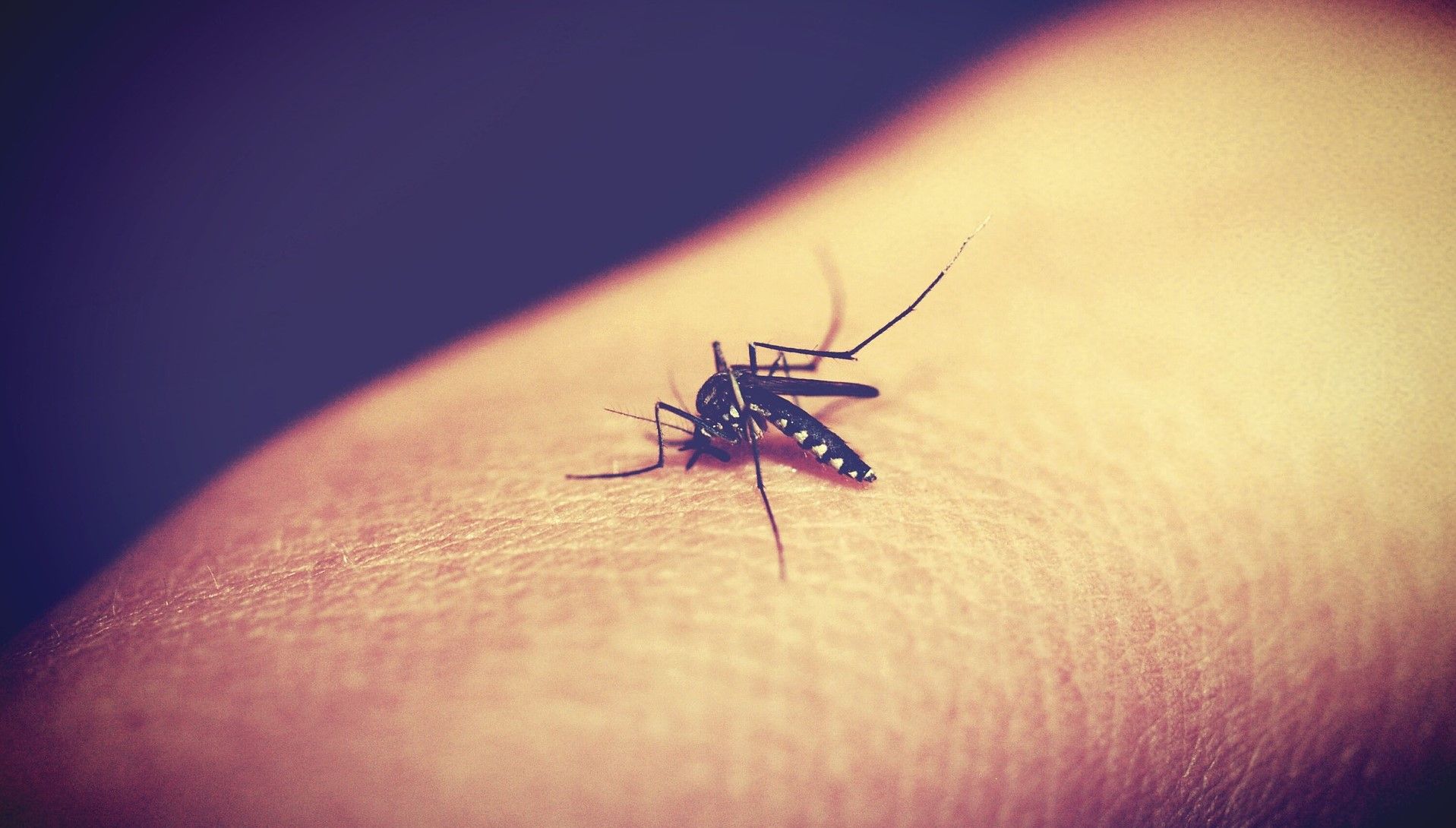
As an infectious disease transmitted by a mosquito-borne parasite, the most common way of malaria transmission is by an infected mosquito bite. At its core, malaria is a parasitic disease responsible for the deaths of at least a million people every year, 90% of whom live in Sub-Saharan Africa. If left unchecked, the disease itself can quickly become life-threatening, usually between 24 to 48 hours. Pregnant women and children are particularly vulnerable. In fact, the greatest death toll occurs in children under five.
In 2017 alone, there were an estimated 219 million cases of malaria reported across 87 countries, with a death toll that stood at 435 thousands. Out of those, 92% of the reported cases and 93% of the deaths were from the African region. Malaria is a preventable and treatable disease. However, despite the effectiveness of the prevention and treatment methods at our disposal, the threat and burden of malaria still remain high. Research illustrates that at least 40% of the world’s population resides in areas considered to be malaria breeding grounds and an estimated one million people die each year from the deadly disease.
Malaria is most entrenched in the poorest countries in the developing world
The reason why the parasite affects young children the most, is because they have yet to develop immunity to it. Besides also affecting pregnant women, research further demonstrates that almost one-fifth of all deaths of children under 5 years old in Sub-Saharan Africa is thought to be due to malaria.
A brief background

Yearly malaria costs in Africa can reach up to USD 12 billion
Many of the world’s poorest nations are severely affected and there is a strong link between malaria and lack of economic growth. It is no coincidence that the only parts of Africa that have experienced or are experiencing reduced rates of malaria are the northern and southern regions – areas that coincidentally harbor the richest countries in the continent. In the Western Hemisphere, the country with the worst malaria, Haiti, also happens to be the poorest one in the region.
Historically, countries with high malaria transmission have had lower economic growth than in countries without malaria. Research illustrates that every year malaria is estimated to cost Africa USD 12 billion in lost Gross Domestic Product (GDP). It is also estimated that malaria has slowed down Africa’s economic growth by 1.3% every year due to loss of life which in turn leads to reduced productivity. For nations with a high malaria burden, the disease may account for as much as 40% of public health expenditure, with malaria accounting for up to 50% of outpatient visits. In Tanzania, for instance, malaria accounts for 30% of the national disease burden. Figures in Tanzania also show that malaria accounts for 43% of under-5-year-olds’ outpatient attendance, 35% of under-5-year-olds’ hospital admissions and 37% of under-5 years olds’ hospital deaths.
The human suffering and loss of life caused by malaria are often matched by the economic burden placed on families who bear the direct costs from their own pockets. Personal expenditure includes spending on insecticide nets, doctors, drugs, and much more. This can put an unbearable strain on household resources. There are also indirect costs for families and households associated with malaria. The permanent neurological and physical damages caused by severe cases of the epidemic tend to disrupt children’s schooling and their general well-being. In turn, this directly affects the children's’ education and ability to earn later in life.
About the Epidemic
Freeing the world of malaria needs greater funding and prevention efforts
From understanding the infection cycle to having the knowledge about prevention methods and options, all steps are important if we want to achieve worldwide eradication in the future. Both go hand in hand with the accessibility of antimalarials for treatment. However, all are extremely dependent on the availability of funding.
Infection
Human infection begins when malaria plasmodium parasites enter a person’s body via a mosquito bite. The parasites then duplicate in the liver before being released into the bloodstream, an action that produces the clinical disease. The resulting symptoms associated with malaria include high fever, sickness, and chills, but the infection can be worsened by organ failure and coma resulting from extreme malaria. Furthermore, if a non-parasitic mosquito bites a person already infected with malaria, it can also become infected and spread the parasite to other people. The effect can be often seen affecting multiple people in a household or village. Learn more about the cycle of malaria transmission in our previous infographic and article here.
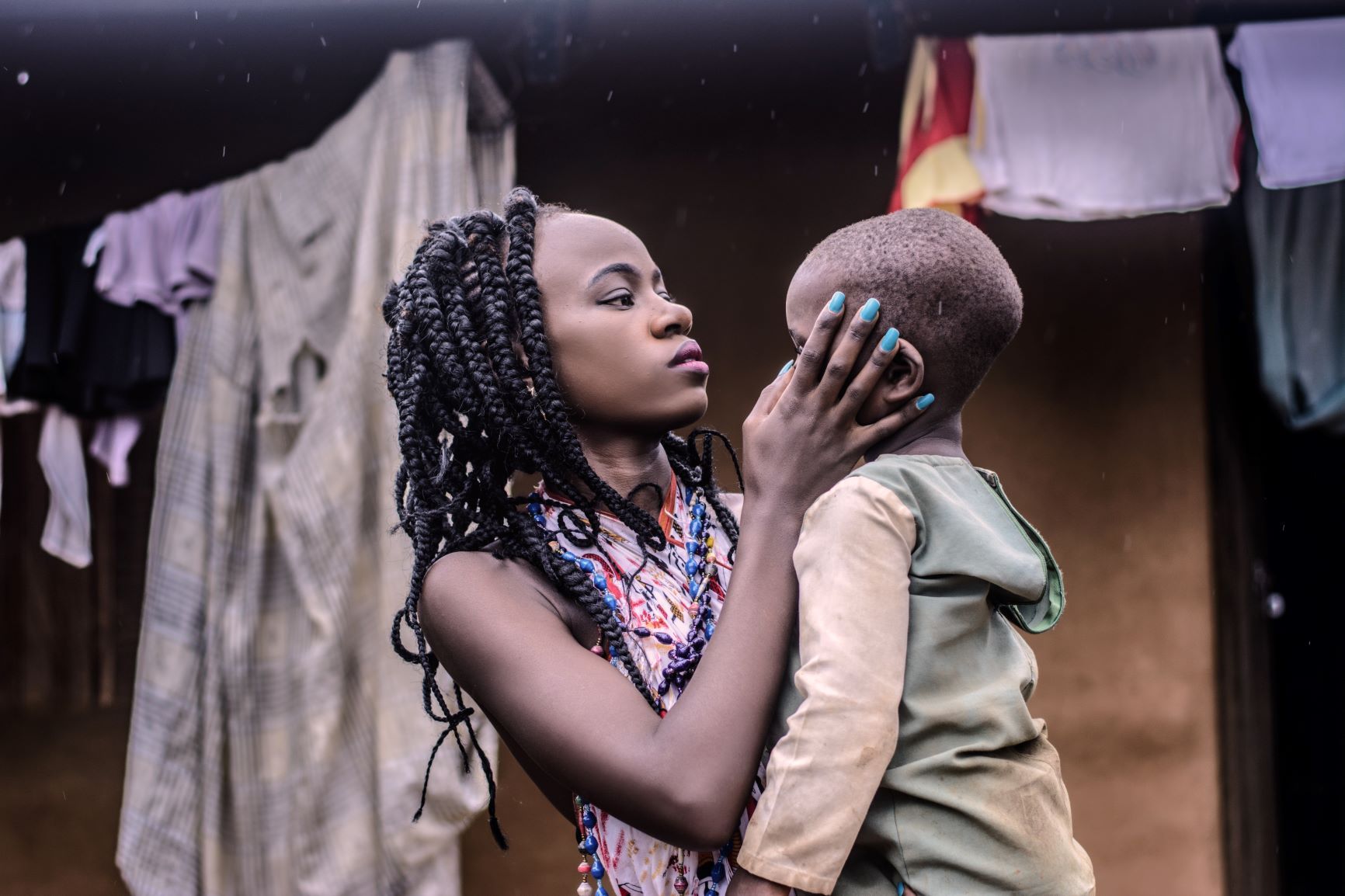
Prevention
As discussed above, the complexity of the epidemic implies that numerous strategies are employed in developing countries for prevention, treatment and eradication of malaria. Methods to prevent malaria for example involve targeting mosquitoes or using pre-emptive treatment. Based on this, there are three most fundamental methods being used:
- Insecticide treated nets (also known as ITNs) which have proven to be very effective in reducing any malaria-related causes of deaths in children under 5 years old. Long-lasting ITNs have recently been promoted by the WHO and Roll Back Malaria partners as a cost-effective and sustainable method for protection against malaria. The more advanced and effective Long Lasting Insecticidal Nets (LLINs) are much more effective as they are treated in the factories with an insecticide incorporated into the net fabric which makes the insecticide last for at least 3 years.
- Indoor Residual Spraying (IRS) of houses and the surrounding environment with approved and effective insecticides. This method has been widely used by developing nations in Asia, the Pacific and Latin America, while in Africa its use has been more restricted to the margins of malaria distribution in Southern Africa plus other nations that are susceptible to epidemics. For IRS to be effective, there needs to be an acute adherence to application procedure, efficacy on the insecticide, public acceptance of spraying, availability of well-maintained equipment, adequately trained spraying personnel, efficient supervision, and strong financial support.
- Antimalarial drugs can also be used in malaria prevention. The available range of antimalarials includes medicine such as chemoprophylaxis, sulfadoxine-pyrimethamine and amodiaquine, mostly used for prevention among travelers visiting malaria-prone regions. Yet, this method of chemo-prevention is also recommended for prevention of seasonal malaria in the Sahel sub-region of Africa.
Funding
With all development aid, there is a need for sustainable and predictable financing so that nations can forecast the amount of money they will receive. Funding for malaria has been extremely unpredictable over recent years. There has been a wide gap in terms of the amount of money needed to make an impact on malaria (estimated at USD 3 billion per year) and the sum contributed by donors (estimated at USD 600 million in 2004, although this figure has since increased).
Most multilateral funding for malaria now goes through the Global Fund to fight AIDS, TB and Malaria, an organization established to increase funds for preventing and treating these diseases. To date, countries such as the UK have pledged more than USD 600 million to the Global Fund in its fight against malaria. Despite international collaboration, there is still a large deficit in aid directed towards malaria. Even with an array of tools available, the global burden of malaria remains very high. In addition to funding issues, there are other barriers to achieving reductions in malaria-related illnesses and deaths.
Treatment and Eradication
In addition to medicines, the first approach to and effective treatment should always be accurate and rapid diagnostic detection. Early diagnosis and treatment not only reduces mortality rate, but also the disease transmission. Malaria test kits are now available for rapid on-site tests. They play an especially important role in rural villages of developing countries, where the nearest healthcare facility might be miles away. Results of parasitological confirmation can be available in 30 minutes or less.
Freeing the world of malaria would be one of the greatest achievements in public health Dr. Tedros Adhanom Ghebreyesus, General Director at WHO
Malaria eradication is defined as the permanent reduction to zero of the worldwide incidence of malaria infection caused by human malaria parasites as a result of deliberate activities. WHO named the countries with at least 3 consecutive years of 0 local malaria cases as eligible for malaria elimination certification. In recent years, 9 countries have been certified by the WHO General Director as having eliminated malaria: United Arab Emirates (2007), Morocco (2010), Turkmenistan (2010), Armenia (2011), Maldives (2015), Sri Lanka (2016), Kyrgyzstan (2016), Paraguay (2018) and Uzbekistan (2018).
According to WHO, eradication of malaria would both save lives and boost economies. By scaling up current malaria interventions, it is estimated that we could prevent an additional of 2 billion malaria cases and 4 million deaths by 2030. This goal can only be achieved if these interventions reach 90% of the population in the 29 countries that account for 95% of the global burden. In the end, although the costs of malaria interventions are high at an estimated US 34 billion, the success of the scale-up will not only even it out but also provide US 283 billion of economic growth in total GDP.
Don't want to miss the next AdvaCare article?
