Blood Transfusion Bag
Material
Type
Volume
Packaging
What is a Blood Transfusion Bag?
Blood Transfusion Bag is a sterile, plastic bag used to collect and store blood and blood products for various medical procedures. It has different types: single, double, triple, and quadruple, and is made of either welding PVC film or blow extruded PVC film. It can hold different blood volumes 250ml to 450ml.
Blood transfusion bags are a critical component of the transfusion process and are used to safely and efficiently deliver blood to patients who require it. Blood bags are also designed with features to help prevent contamination during the collection and storage process, such as sterile ports and tamper-evident seals.
This Blood Transfusion Bag is manufactured by AdvaCare Pharma at ISO and CE certified facilities located in India, China, and the USA. Our facilities are regularly inspected to ensure compliance with all healthcare standards for quality and safety.
Product Specifications
Material
Type
Welding PVC Film
Welding PVC film blood transfusion bags are manufactured using a process that involves welding and cutting two layers of PVC film together. This is achieved through ultrasonic, high-frequency, or NWS (pulse/thermal) welding methods. The resulting bags are sterile, durable, and reliable for the safe storage and transfusion of blood and blood products.
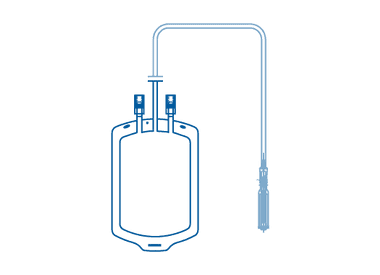
Blown Extruded PVC Film
Blown Extruded PVC Film blood transfusion bags with a tubular shape are made using a blown extrusion process that results in seamless edges without the need for welding. This method involves extruding PVC film through a circular die and then inflating it to the desired size and shape. The resulting bags are strong, flexible, and ideal for safe storage and transfusion of blood and blood products.
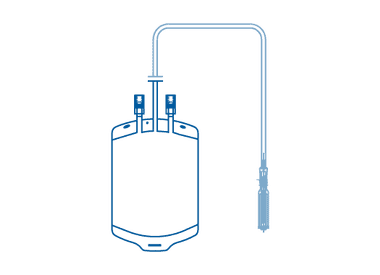
Single
Single blood transfusion bags are designed for the collection, processing, and transfusion of whole blood. These blood collection bags contain CPDA-1 solution, a common anticoagulant and nutrient solution used in blood banking. With their sterile and reliable design, single blood bags are a trusted option for safe and effective transfusion procedure.
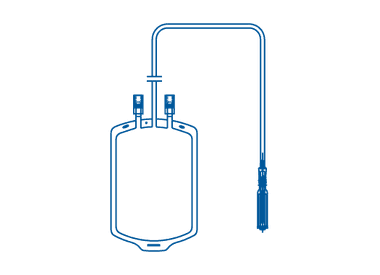
Double
Double blood transfusion bags are designed for the collection of whole blood and the separation of two different blood components (red blood cells and plasma) through the process of centrifugation and extraction. These bags feature two compartments that allow for the separate storage and transfusion of each component, providing a safe and effective method for blood transfusion.
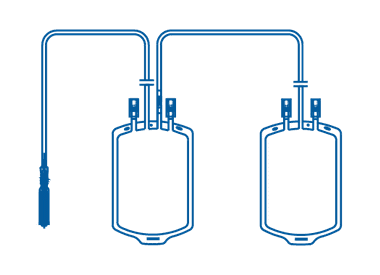
Triple
Triple blood transfusion bag is specially designed for whole blood collection, processing, and transfusion. This type of blood bag contains CPDA-1 and SAGM (Saline-Adenine-Glucose-Mannitol) solutions for the separation of three different blood components, namely red blood cells, plasma, and a buffy coat comprising leukocytes and platelets, which are obtained through centrifugation and extraction.
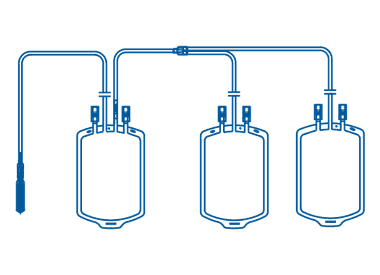
Quadruple
Quadruple blood transfusion bag is specially designed for whole blood collection and separation into four different components: red blood cells, plasma, leukocytes, and platelets. This separation is achieved through the process of centrifugation and extraction, providing a safe and effective solution for medical procedures that require blood transfusion and/or separation.
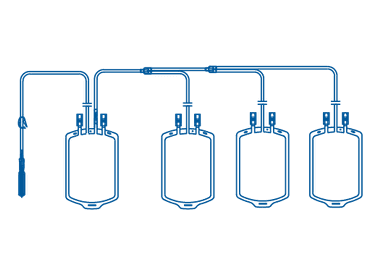
Why choose us as your Blood Transfusion Bag manufacturer?
AdvaCare Pharma is a reliable manufacturer of Blood Transfusion Bags, which come in different materials, volume capacities, and types. Our AccuPoint™ brand products are supported by a STED dossier, and our manufacturing facilities, located in China, India and USA, comply with stringent ISO and CE certifications. We conduct frequent internal and third-party facility evaluations to guarantee that all medical devices under our brand meet and exceed the standards required by our distributors.
We are a quality blood bag manufacturer founded on the premise of providing the best value to medical distributors by focusing on high quality, affordable products and market-specific solutions. As a supplier of medical devices for over 20 years, we have implemented a vested supplier-distributor relationship to set us apart from any other large scale medical manufacturer with global distribution. Our current distribution network spans 65 markets worldwide.
Uses
How should a Blood Transfusion Bag be used in healthcare settings?
Blood Transfusion Bags are invaluable across various medical settings, from hospitals to clinics and larger healthcare institutions. They enable the direct delivery of blood and its components through intravenous methods to those in need. This method is pivotal in a myriad of medical treatments, providing a streamlined approach to transfusions.
Hospitals widely use these blood transfusion bags for a range of activities, from routine examinations to care in the emergency department. Clinics depend on them for extracting blood samples for diverse tests, thus positively impacting the patient experiences, especially with the aid of devices like the AccuPoint™ series. The flexibility of these bags is highly valued in medical centers for numerous services, including blood donations and detailed diagnostic evaluations.
How should a Blood Transfusion Bag be used by healthcare professionals?
Skilled professionals such as doctors, nurse practitioners, and phlebotomists undertake the careful application of Blood Transfusion Bags. Their expertise is foundational in maximizing patient comfort, reducing the potential complications, and obtaining precise laboratory results. The selection of an appropriate bag, taking into account the specific needs of the patient and the procedure, is required for successful outcomes.
How should a Blood Transfusion Bag be disposed of to comply with safety standards?
Following the use of Blood Transfusion Bags, their disposal becomes a priority to maintain health standards and comply with regulations. These bags, once utilized, require handling in accordance with strict biomedical waste protocols. Placement in designated biohazard containers underscores the need for meticulous disposal procedures, safeguarding healthcare workers, patients, and the environment from potential risks.
What safety precautions should healthcare professionals take when using Blood Transfusion Bags?
When handling Blood Transfusion Bags, it is imperative for medical personnel to rigorously follow established safety guidelines. This detailed protocol involves wearing protective gloves, masks, and eye protection to minimize exposure to bloodborne pathogens, a measure that's non-negotiable in safeguarding both staff and patients.
Emphasizing comprehensive hygiene practices stands as a cornerstone of safe handling procedures. This includes thorough handwashing and the meticulous application of sterile techniques throughout every step of the procedure. By doing so, healthcare workers substantially reduce the likelihood of contamination, thereby raising the standards of patient care and creating a safer environment for both the providers and recipients of medical services.
What are the common complications and challenges associated with using Blood Transfusion Bags?
Navigating the challenges and the potential complications associated with Blood Transfusion Bags requires vigilance from healthcare professionals. These include issues such as achieving vein access, managing transfusion reactions, and avoiding fluid imbalances.
FAQs
What is the difference between Blood Transfusion Bags made of welding PVC film and blown extruded PVC film?
The main difference is the manufacturing process. Welding PVC film blood bags are made by welding together two sheets of PVC film, while blown extruded PVC film blood collection bags are made by blowing air into a cylinder of molten PVC to create a tube. Additionally, welding PVC film tends to have a smoother surface and is more transparent, while blown extruded PVC film is more flexible and has better puncture resistance.
What are the differences between single, double, triple, and quadruple Blood Transfusion Bags?
Single blood transfusion bags are designed to collect and store one unit of whole blood or a blood component, while double bags can store two units. Triple bags can store three units, and quadruple bags can store four units. The bags are designed with different compartments to allow for the separation and preservation of different blood components such as red blood cells, plasma, platelets, and cryoprecipitate.
How is a Blood Transfusion Bag prepared and stored?
Before use, the blood transfusion bag is prepared by a healthcare professional, who will verify the blood type and compatibility of the blood product and attach a label with the patient's information. The bag is then stored in a designated area, such as a refrigerator or blood bank, until it is ready to be used. It is important to follow proper storage and handling procedures to ensure the safety and efficacy of the blood product.
Can Blood Transfusion Bags be reused or recycled?
Blood transfusion bags are single-use medical devices and should not be reused or recycled. Reusing or recycling blood transfusion bags can lead to contamination and compromise the safety of the blood product. After use, the bag should be properly disposed of according to local regulations and guidelines.
How are Blood Transfusion Bags tested for safety and quality?
Blood transfusion bags undergo extensive testing and quality control measures to ensure their safety and efficacy. The bags themselves are tested for leaks, cracks, and other defects to ensure that they are sterile and intact. In addition, the bags are subjected to a variety of physical and chemical tests to verify that they meet the necessary specifications for strength, durability, and compatibility with blood products.
Is regulatory support available for importing your Blood Transfusion Bags?
We offer extensive regulatory support to our distributors, aiding in navigating local regulations and facilitating the importation of our medical devices. With the expertise of our Regulatory Affairs Department, which includes qualified professionals such as pharmacists, biomedical engineers, QA specialists, and documentation experts, we ensure a seamless product registration experience.
Do your Blood Transfusion Bags meet CE certification requirements?
Certainly, our medical devices meet CE certification standards, ensuring compliance with European Union regulations. Furthermore, our manufacturing protocols strictly adhere to ISO standards to maintain high-quality standards across all products.
What are the difficulties associated with importing Class II medical devices for distribution?
Importing Class II medical devices may require navigating more stringent regulatory requirements, yet with proper documentation and compliance, it is feasible. Our Regulatory Affairs Department supports distributors in efficiently registering Class II devices in their target markets.
References
Shelf-life and Performance of Blood Bags
A study in Scientific Reports examines the properties of SEBS/PP polymer blend blood bags compared to traditional PVC-DEHP bags. It focuses on essential characteristics such as weld strength, oxygen and water permeability, and shelf life, ensuring these materials are suitable for blood storage.
Properties and Uses of PVC Blood Bags
PVCMed Alliance highlights the advantages of PVC blood bags, emphasizing their durability, extended shelf life, sterility, and cost-effectiveness. These bags have been crucial in blood storage and transportation since their inception before 1950, enhancing medical practices.



